Respiratory health begins with clarity, and that clarity often comes through objective testing. As Sushil Gupta, MD, has emphasized through years of pulmonary practice, sleep apnea cannot be effectively treated without first understanding exactly how it presents in the individual patient. A sleep study is not simply a formality; it is the foundation of accurate diagnosis and long-term respiratory protection.
Sleep is often misunderstood as a passive state. In reality, it is one of the most physiologically active periods for the body. Breathing patterns shift, oxygen levels fluctuate, heart rate adjusts, and muscle tone changes. For individuals with obstructive sleep apnea (OSA), these natural shifts can trigger repeated airway collapse, oxygen deprivation, and stress responses that occur dozens, sometimes hundreds, of times per night.
Without proper testing, these disruptions remain invisible.
Why Symptoms Alone Are Not Enough
Snoring, daytime fatigue, morning headaches, and difficulty concentrating are common warning signs. Yet symptoms vary widely. Some patients experience severe apnea with minimal perceived fatigue, while others feel exhausted but have milder obstruction. This variability is why guesswork fails.
A sleep study, formally known as polysomnography, measures critical physiological data during sleep, including:
- Brain wave activity
- Blood oxygen levels
- Heart rate and rhythm
- Respiratory effort
- Airflow
- Limb movement
These measurements uncover patterns that are not detectable during a typical office visit. Importantly, they quantify the apnea-hypopnea index (AHI), which determines the severity of sleep apnea and guides treatment decisions.
Accurate numbers matter. Mild, moderate, and severe cases require different management approaches.
What Happens During a Sleep Study
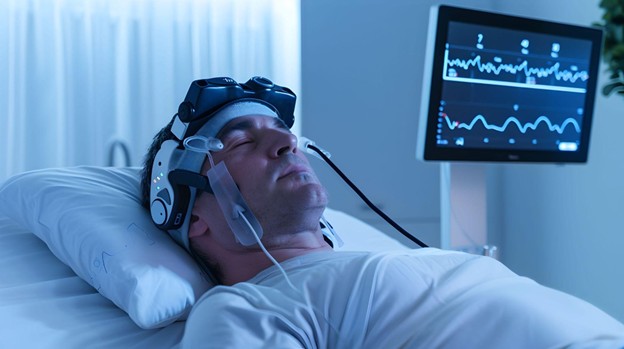
Many patients delay testing because they imagine it to be uncomfortable or invasive. In reality, modern sleep labs are designed to resemble comfortable bedrooms. Sensors are placed on the scalp, chest, and limbs using adhesive pads. A small nasal cannula monitors airflow, and a pulse oximeter measures oxygen saturation.
Patients then sleep while data is recorded throughout the night.
Technicians monitor the study remotely, ensuring accuracy and safety. The result is a detailed map of how the body performs during rest, revealing interruptions that might otherwise go undetected for years.
For certain patients, home sleep apnea testing (HSAT) may be appropriate. These simplified devices track airflow, oxygen levels, and respiratory effort. While not suitable for every case, home testing has expanded access to diagnosis for many individuals.
The Hidden Cost of Delayed Diagnosis
Untreated sleep apnea is not just a nighttime issue. It has measurable consequences across multiple organ systems.
Repeated oxygen drops strain the cardiovascular system. Each pause in breathing triggers a stress response that elevates blood pressure and heart rate. Over time, this pattern increases the risk of:
- Hypertension
- Atrial fibrillation
- Coronary artery disease
- Stroke
- Type 2 diabetes
Cognitive health is also affected. Chronic sleep fragmentation impairs memory, attention, and mood stability. Many patients initially attribute these symptoms to aging or work stress, unaware that sleep-disordered breathing is the underlying cause.
Early sleep studies interrupt this progression. They replace uncertainty with data and allow physicians to intervene before complications escalate.
The Role of Pulmonary Expertise
Sleep apnea intersects directly with pulmonary medicine because airway mechanics and lung function influence breathing stability during sleep. Individuals with asthma, chronic obstructive pulmonary disease (COPD), obesity, or restrictive lung disease may experience more complex sleep-disordered breathing patterns.
Pulmonary evaluation alongside sleep testing ensures that contributing respiratory factors are addressed. This integrated approach strengthens outcomes and reduces recurrence.
Testing is not simply about identifying apnea; it is about understanding why it occurs in that specific patient.
Moving Beyond a One-Size-Fits-All Approach
Once a sleep study confirms diagnosis and severity, treatment planning begins. Continuous positive airway pressure (CPAP) continues to be the most effective treatment for moderate to severe obstructive sleep apnea. However, therapy must be tailored.
Pressure settings are often determined during a titration study, which identifies the precise airflow needed to prevent airway collapse. In some cases, bilevel devices, oral appliances, positional therapy, or weight management strategies may be recommended.
Without initial diagnostic accuracy, treatment becomes trial and error.
With proper testing, therapy becomes targeted and measurable.
Objective Data Drives Long-Term Success
Sleep apnea is a chronic condition for many individuals. Ongoing management requires measurable benchmarks. Sleep study results serve as a reference point for evaluating improvement, adjusting devices, and tracking health outcomes.
Follow-up studies may be performed if symptoms change or weight fluctuations occur. In this way, sleep testing becomes part of a broader respiratory health strategy rather than a one-time event.
This long-term perspective is critical because untreated or inadequately treated apnea often returns quietly.
Breaking the Cycle of Underdiagnosis
Despite increased awareness, millions of individuals remain undiagnosed. Cultural normalization of snoring and fatigue contributes to the delay. Many people assume disrupted sleep is inevitable in midlife.
It is not.
Education about the value of sleep studies helps dismantle these assumptions. Objective testing removes stigma and replaces it with clarity. For employers, families, and communities, improved sleep health translates into better concentration, safer driving, and stronger cardiovascular outcomes.
Precision Over Assumption
Healthcare increasingly favors data-driven decision-making. Sleep medicine is no exception. Relying solely on symptom descriptions can overlook silent hypoxia or underestimate severity. Polysomnography transforms subjective complaints into measurable evidence.
For patients who have struggled with unexplained fatigue or persistent snoring, testing often provides relief simply by naming the problem. A clear diagnosis empowers action.
The First Step Toward Restorative Sleep
Treating sleep apnea effectively begins with understanding its full physiological footprint. A comprehensive sleep study does more than confirm a suspicion; it reveals patterns that guide personalized intervention and protect long-term pulmonary and cardiovascular health.
Accurate testing is not an optional step. It is the starting point.
When patients prioritize diagnostic clarity, they invest not only in better sleep but in sustained respiratory strength and overall wellness for years to come.